Your top news on business and economy
Provided by AGPRoboCT Welcomes Peer-Reviewed Study on Exoskeleton Gait Rehabilitation After Stroke
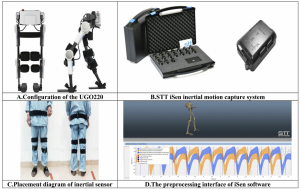
Experimental setup showing the UGO220 exoskeleton, STT iSen sensors, sensor placement, and gait analysis software.
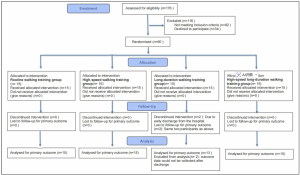
CONSORT Flow Diagram. Participant enrolment, randomisation, allocation, follow-up, and analysis across the four exoskeleton-assisted walking training groups.
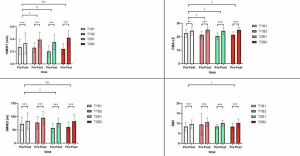
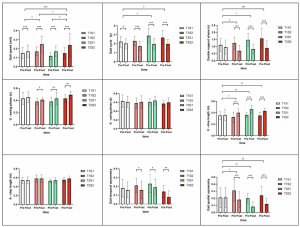
Comparison of Clinical Outcomes. Pre- and post-intervention changes in 10MWT, FMA-LE, 6MWD, and RMI across the four exoskeleton-assisted walking training groups.
Peer-reviewed study supports a more evidence-based approach to exoskeleton-assisted gait rehabilitation after stroke.
The study, titled “Effects of different intensity training with a lower limb exoskeleton robot on walking function in people with subacute stroke: a randomized controlled trial,” used the UGO220 Exoskeleton Robot System and compared four fixed training regimens based on two clinically relevant variables: robot-assisted walking speed and single-session training duration. The study was conducted with people with subacute stroke at Shanghai Yangzhi Rehabilitation Hospital between January and November 2024 and was published online on 19 March 2026.
For RoboCT, the significance of the publication lies not only in the reported clinical outcomes, but in the broader direction it represents for rehabilitation robotics. As robotic rehabilitation technologies become increasingly adopted in hospitals and rehabilitation centres, the next stage of clinical progress will depend on better answers to a more precise question: not simply whether robotic gait training can be useful, but how robotic training should be prescribed, dosed, monitored and adapted for different patient needs.
“Rehabilitation robotics must move beyond hardware demonstration and toward evidence-informed clinical protocols,” said Dr Wang Tian, Founder and CEO of RoboCT. “This study is meaningful because it evaluates specific training parameters — speed and duration — in a structured way. It helps clinicians, researchers and technology developers think more carefully about how robotic gait training can be delivered with greater precision, consistency and clinical discipline.”
Addressing a major rehabilitation challenge after stroke
Stroke remains one of the world’s most significant causes of death and disability. The World Stroke Organization’s 2025 Global Stroke Fact Sheet states that stroke is the second leading cause of death and the third leading cause of death and disability combined globally; it also estimates the global cost of stroke at more than US$890 billion.
Walking impairment is one of the most common and functionally important consequences of stroke. The newly published study notes that approximately 80% of people with stroke experience walking dysfunction, and many continue to experience walking difficulties months after the event. The first three to six months after stroke are widely recognised as a critical window for rehabilitation intervention, making effective, intensive and well-structured gait rehabilitation especially important.
Conventional rehabilitation remains essential, but clinical teams often face time, resource and staffing constraints that make it difficult to deliver sufficient repetition and intensity. Lower-limb exoskeleton robots can help address this challenge by providing quantifiable, repeatable and parameter-driven walking training under professional supervision.
The UGO platform is designed for use in hospitals and rehabilitation departments for people with lower-limb motor dysfunction, with features including intent detection, standard gait training, bionic design and cloud-based rehabilitation assessment support. RoboCT’s official product information describes UGO as a medical-use exoskeleton intended to support ambulatory training in rehabilitation and medical institutions.
From device adoption to protocol optimisation
The newly published study is important because it directly addresses a gap in the rehabilitation robotics field: the lack of standardised evidence on training parameters.
Although exoskeleton-assisted gait training has been studied across different stroke populations and device types, many studies vary widely in session duration, training frequency, walking speed and patient selection. A 2024 systematic review and meta-analysis of lower-limb robotic exoskeleton training in stroke found that such training can improve lower-limb function, gait parameters, activity and participation outcomes, but also highlighted the need for more detailed analysis of training intensity, device type and stroke phase.
The new randomised study builds on this gap by using a 2×2 factorial design to compare two walking speeds and two session durations:
+ Routine speed and routine duration: 0.2 m/s for 20 minutes
+ High speed and routine duration: 0.5 m/s for 20 minutes
+ Routine speed and long duration: 0.2 m/s for 50 minutes
+ High speed and long duration: 0.5 m/s for 50 minutes
All groups also received the same 40 minutes of conventional rehabilitation and underwent exoskeleton-assisted gait training five sessions per week for three weeks, for a total of 15 sessions. This design allowed the researchers to examine whether speed, duration, or the combination of both appeared to influence different aspects of walking recovery.
Study design and assessment approach
The trial was designed as a randomised, assessor-blind, parallel-group controlled study with an exploratory framework. Sixty people with subacute stroke were enrolled and randomly assigned to four groups using a computer-generated allocation sequence. Fifty-eight participants completed the study; two participants withdrew due to discharge and return home, not because of exoskeleton-related intolerance or adverse reactions.
The study assessed both clinical and biomechanical outcomes. Clinical measures included the 10-Metre Walk Test, Fugl-Meyer Assessment of Lower Extremity, 6-Minute Walk Distance*, and Rivermead Mobility Index. Spatiotemporal gait parameters included gait speed, gait cycle time, double support phase time, swing phase time, step length and gait asymmetry.
This combination of outcome measures is important because walking recovery after stroke is multidimensional. A patient’s progress cannot be fully understood through walking speed alone. Clinicians also need to understand motor control, endurance, gait symmetry, compensatory movement patterns and the patient’s ability to translate walking improvements into daily activity and participation.
Key findings: intensity parameters may matter
The study reported significant improvements in all four clinical outcome measures across all groups after intervention. Between-group comparisons showed statistically significant differences in 10-Metre Walk Test performance, lower-extremity motor function, 6-Minute Walk Distance and Rivermead Mobility Index. In post-hoc analysis, the high-speed group, long-duration group and high-speed plus long-duration group showed greater improvements than the routine-speed, routine-duration group in selected outcomes.
The most notable finding was that the high-speed plus long-duration protocol showed the strongest overall pattern of improvement among the tested regimens. The study reported that this group demonstrated the greatest improvement in gait speed and outperformed the routine-speed, routine-duration group in daily activity and participation as measured by the Rivermead Mobility Index.
The authors also examined Minimal Clinically Important Difference thresholds. According to the study, only the high-speed plus long-duration group reached the MCID threshold for the 10-Metre Walk Test, while the high-speed, long-duration and combined high-speed plus long-duration groups reached clinically significant improvement in gait speed. For walking endurance, only the high-speed plus long-duration group clearly exceeded the 20-metre MCID threshold for the 6-Minute Walk Distance.
Taken together, these findings suggest that walking speed and training duration should not be treated as interchangeable variables. Speed may be particularly relevant to walking velocity and gait quality, while duration may be particularly relevant to endurance. Their combination may provide a stronger total training dose for selected patients under appropriate clinical supervision.
Safety findings under professional supervision
The study reported that all exoskeleton-assisted interventions were delivered under the close supervision of professional rehabilitation therapists. No serious adverse events occurred among the 58 participants who completed the study. Non-serious adverse events occurred in 17.2% of participants and were described as mild, including fatigue, transient dizziness, calf muscle soreness and one case of skin erythema at the exoskeleton wearing site that was relieved by strap adjustment. No participant withdrew due to adverse events or poor tolerance.
RoboCT emphasised that these findings should be interpreted responsibly. The safety findings relate to a structured clinical trial conducted in a professional rehabilitation environment, with defined eligibility criteria, therapist supervision, adverse-event monitoring and training suspension rules.
“This is an important point,” said Wang. “The study should not be read as a general recommendation for unsupervised high-intensity training. The higher-intensity protocol was delivered in a controlled clinical setting by trained rehabilitation professionals. That distinction matters for patient safety, clinical governance and responsible communication.”
The role of UGO220 in parameter-driven rehabilitation
The UGO220 Exoskeleton Robot System used in the study is described in the paper as a ground-based wearable device designed to support lower-limb walking function in patients with walking dysfunction. The paper describes several core system characteristics, including ergonomic bionic design, motion-intention detection, assisted torque output, parameter-driven torque curve generation and cloud-based intelligent rehabilitation management.
In the trial, the UGO220 system used preset walking speeds and step length settings to generate corresponding hip and knee joint assistive torque curves. Therapists were responsible for correct device wearing, parameter setting and safety monitoring, while manual adjustment of core gait-assist parameters during the intervention was not permitted.
This parameter-driven approach is important because it supports repeatability. In clinical rehabilitation, one of the persistent challenges is the variability of intervention delivery across therapists, centres and patient groups. Robotic systems can help standardise aspects of gait training while preserving the central role of clinicians in assessment, decision-making, supervision and progression.
A measured interpretation: evidence-supported, not overclaimed
RoboCT believes the study provides valuable clinical evidence, but the company is careful not to overstate its implications. The study supports the relevance of structured parameter testing in exoskeleton-assisted gait rehabilitation after subacute stroke. It does not mean that a single protocol is universally optimal for all stroke patients, nor does it establish long-term outcomes across all settings.
The authors themselves identified several limitations. The intervention lasted 15 sessions, and no long-term follow-up was conducted. The study was conducted at a single centre with a limited sample size, and the findings primarily apply to hospitalised patients in the subacute phase of stroke recovery. Participants and therapists could not be blinded due to the nature of the intervention. The device was tested at only two walking speed levels, with a maximum speed of 0.5 m/s, which limited assessment of higher-speed protocols.
For this reason, RoboCT will describe UGO220 as having been used in a peer-reviewed randomised clinical study, rather than making broad claims of universal clinical validation. The company views the publication as part of an accumulating evidence base that can inform future research, clinical collaboration and protocol development.
Scientific credibility comes from precision,” said Wang. “The strongest message is not that one device solves stroke rehabilitation. The stronger message is that robotic rehabilitation can become more clinically useful when it is studied through dosing, protocol design, patient stratification and measurable outcomes. That is how the field matures.”
Implications for clinicians and rehabilitation centres
For clinicians, the study offers practical insights into how different rehabilitation goals may require different robotic training parameters. Patients with poorer walking ability may benefit from prioritising longer-duration training to build endurance, while patients with better baseline walking ability may benefit from higher-speed training to improve walking speed and gait quality. The study’s conclusion suggests that the combined high-speed and long-duration protocol appeared preferable among the tested combinations, while also recognising the need for individualisation.
For rehabilitation centres, the findings reinforce the importance of clinical workflow design. Robotic systems are not simply equipment purchases; they are clinical platforms that require therapist training, patient selection, safety procedures, data collection and protocol governance. The value of rehabilitation robotics depends on how effectively it is integrated into clinical pathways.
For researchers, the study points toward the need for larger, multicentre trials with longer follow-up periods, broader patient populations, and more granular intensity settings. Future studies may also examine how exoskeleton-generated data can support personalised rehabilitation progression, identify responders and non-responders, and link gait laboratory outcomes with real-world participation.
RoboCT’s evidence-led direction
RoboCT specialises in the research, development and application of exoskeleton robotics, providing intelligent products and customised solutions for medical institutions and individual users. The company’s official materials describe its focus on exoskeleton technology across healthcare and other sectors, and its product portfolio includes UGO, UFU, URA and KidGo systems for medical and rehabilitation applications.
As the rehabilitation robotics industry evolves, RoboCT aims to support a more evidence-led model of adoption. This means working with clinicians, hospitals, rehabilitation centres and researchers to understand not only what robotic systems can do, but how they can be used safely, appropriately and effectively within real clinical pathways.
“The future of rehabilitation robotics will be defined by evidence, integration and clinical trust,” said Wang. “This publication is an encouraging step because it contributes to a more disciplined conversation about training design. RoboCT will continue to support research, clinical collaboration and responsible communication so that robotic rehabilitation can serve patients and clinicians with greater confidence.”
Publication and responsible use of study materials
The article is available as an open-access publication in the *Journal of NeuroEngineering and Rehabilitation*. RoboCT will ensure that any external communication about the study accurately reflects the published findings and limitations. Figures, charts, tables or images from the article will not be used in commercial materials unless the appropriate publication rights and permissions are confirmed.
About RoboCT
RoboCT Technology Development Co., Ltd. is an exoskeleton robotics company focused on the research, development and application of intelligent robotic systems for rehabilitation, healthcare and related fields. RoboCT develops exoskeleton products and customised solutions for medical institutions, rehabilitation providers and individual users, with a focus on improving mobility support, rehabilitation training and data-enabled clinical workflows.
Media Contact
RoboCT International Business Team
Website: www.roboct.com
Email: wangxiaoqi@roboct.com
Leo Wang
RoboCT
+86 566 375 9821
wangxiaoqi@roboct.com
Scientific and clinical communication note: Source: https://link.springer.com/article/10.1186/s12984-026-01948-1
The UGO220 was used in a peer-reviewed randomised clinical study involving people with subacute stroke. The study findings should not be interpreted as a universal claim of efficacy across all stroke populations, all rehabilitation stages or all care settings. Exoskeleton-assisted gait training should be delivered under appropriate professional assessment, supervision and clinical governance.
Leo Wang
RoboCT
+86 566 375 9821
email us here
Legal Disclaimer:
EIN Presswire provides this news content "as is" without warranty of any kind. We do not accept any responsibility or liability for the accuracy, content, images, videos, licenses, completeness, legality, or reliability of the information contained in this article. If you have any complaints or copyright issues related to this article, kindly contact the author above.